I have a daughter. She just turned two. She is the love of my life. She is cute and precious and just absolutely lovable. I cannot imagine what it would be like if she were to die at any age, but especially at this age or younger. I really could not imagine if I or someone else were accused of killing her by way of Shaken Baby Syndrome (“SBS”). Without a doubt there are very few topics that bring out more understandable passion than child abuse or the death of a child. The fact finder, whether it is a Judge or a Jury, does not have the luxury of passion, but is sworn to examine the evidence critically, with skepticism and analytically.

The typical case involves an infant, one year old or less, who is seen with respiratory distress at the home, then sent to the hospital. The presentation is typically remarkable with notes of subdural hemorrhages with retinal bleeding, no external trauma and no report of a noteworthy fall.
First let’s talk about the current prosecution-oriented myths that surround Shaken Baby Syndrome. Then, we will employ basic and valid biomechanics and generally accepted principles of anthropometry to reality in order to expose these myths.
Well first, let’s take a look at the “loaded language” inherent in the diagnosis. It is called Shaken Baby Syndrome, which evokes quite a bit of emotion based simply upon its title. However, it is now being reframed as Shaken Baby Impact Syndrome, Non-Accidental Injury Syndrome, and Infant Brain Injury Syndrome to exacerbate the cognitive prejudicial effect of it all.
There are several basic myths that underscore and characterize the situation.
The diagnosis is truly a clinical one and not one that is born of any measure of meaningful empirical testing. The notion that the triad or constellation of injuries together can only manifest based upon violent shaking that is intentional to the exclusion of everything else leads to the potential of extreme mistakes.
- Doctors who seek to diagnosis SBS look at several presentation-symptoms during a physical examine to include:
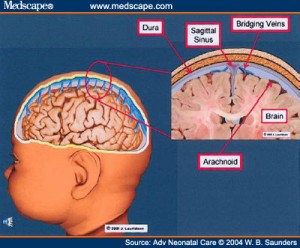
- subarachnoid hemorrhage. (Arachnoid hemorrhage is blood beneath the arachnoid area of the brain. The bridging vein connects the dural sinus to the cortical surface of the brain);
- subdural hematoma. (A subdural hematoma is diagnosed when there is bleeding between the dural covering of the brain into the potential space which usually has no bleeding there);
- patechial retinal hemorrhaging;
- hypoxia;
- the lack of lucid interval between alleged shaking and treatment or examination;
- whether or not the caregiver posits a reasonable explanation according to the treating physician to account for all of this. In other words, does the examining physician believe the caregiver’s explaination for how the damage was sustained?
- The second myth is that the symptomology cannot present itself from a short distance fall of two to three feet.
According to the prosecution, it is the rotational acceleration of the cranium that ruptures these bridging veins and causes subdural hematoma or subarachnoid bleeding and the retinal bleeding.
Now let’s speak the truth. Is it true that after a short distance fall that presents with no outward trauma that there can never be a subdural hematoma or subarachnoid bleeding and the retinal bleeding with no lucid interval?
Well, no.
The best example of the lucid interval between a short distance fall with subdural hematoma or subarachnoid bleeding and the retinal bleeding with no outward trauma was the case of Natasha Richardson. The untimely and unfortunate death of the famous actress occurred when she was on the “bunny hill” during a very short fall at very low impact resulting in no outward trauma. She remained lucid for quite a while afterwards and then died.
Now let’s use basic anthropometry and basic biomechanics to examine whether or not shaking a baby to cause enough rotational injury resulting in these injuries is indeed even possible without resulting in outward trauma?

Well, again, the answer is no.
The most telling physical realities that confronts Shaken Baby Syndrome and reveals it as an unproven belief or at worst a dangerous myth occurs when one scientifically examines this notion that the only explanation when there is a subdural hematoma or subarachnoid bleeding and the retinal bleeding without outward obvious trauma is SBS. There can, in fact, be subdural hematomas or subarachnoid bleeding and retinal bleeding without outward obvious trauma other than from SBS.
In order to prove this is not unique to SBS or to establish that SBS is indeed impossible without outward trauma, we must first know that scientifically there are generally two different types of force: linear force and translational force. The former is a measure of acceleration that always acts in a particular direction, such as gravity. The latter is a measure of acceleration based upon a rotation. In order for there to be sufficient rotational inertia to cause the intracranial injuries in an infant, according to proponents of Shaken Baby Syndrome, there must be between 6000 to 7000 radians per second squared of rotational acceleration exerted on the cranial cavity.
A peer-reviewed study performed on Penn State Division One football players dispels this as a real possibility. They were given a CRABI device[i] and asked to shake the device as violently as possible with the stated aim for these well-trained athletes to create as much rotational force as possible. At their best, they could only generate approximately 1500 radians per second squared. However, when they were asked to slam the child’s head against a hard object, like a floor, they could generate 50,000 radians per second squared. As the researcher noted with this modified method of slamming the child’s head against the floor, an examining physician would see signs of external trauma. This is basically what we would expect to see if the impulse (J) was low. (J = FΔt; as t (deceleration) gets smaller, the J value drops significantly even when presented with the same force. Small J means the change in momentum is very fast, which is obviously going to have physical ramifications. When the experiment was modified to include a short distance fall, sufficient radians per second squared were created.

Further the study found that in order for the football players to generate the approximate 1500 radians per second squared, the players instinctively held on to the rib area so strongly that it would very likely cause broken or bruised ribs and/pr a long bone fracture for example in the arm or leg.
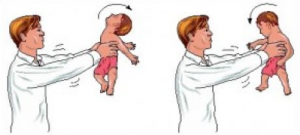
Additionally from the world of biomechanics and anthropometry we learn that in an infant the head is a disproportionately large amount of mass as compared to a human with massively underdeveloped neck musculature to support its weight or orientation. This is why we are all taught to hold a baby’s head when picking it up or the head will flop causing injury to the neck. Such is the case with SBS. If it is an alleged SBS situation, the delicate area of a baby’s neck would definitively present to the examining physician with unmistakable signs of trauma.
Additionally, if there is a lack neck injury then there is also less then demonstrable evidence of Shaken Baby Syndrome as the head and the musculature around the neck of an infant is the most vulnerable area involved with babies.
Other myths that are easily demystified include:
- retinal hemorrhaging is exclusive to abuse (N.B., The true mechanism that causes retinal hemorrhaging is not known)
- subdural hematomas are a presentation of shaking
- retinal bleeding is diagnostic of abuse
- it is impossible to have a period of lucidity afterwards
- chronic subdural hematomas never re-bleed, meaning if there is a preexisting injury then it always heals and it is never subject to re-presentation (N.B., subdural hematomas cannot be dated)
[i] The Child Restraint/Air Bag Interaction (CRABI) dummy has been developed at First Technology Systems, Inc. (FTSS) to evaluate small child restraint Systems in automotive crash environments, in all directions of impact, with or without air bag interaction. There are three sizes of infant dummies: a 6-month-old, 12-month-old, and 18-month old. Accelerometers are used to measure head, chest acceleration and head angular acceleration.



Nina says:
I was wondering what the likliness of shaken baby in an 18 month old baby is and at that age wouldnt there be more likliness of brusing, due to the graps of the person shaking? I also was wondering how would you tell the differance between shaken baby and a baby (18 month old) with water on the brain? If you could clear this up for me I would greatly appreciate it!!
Joe Burns says:
This is an excellent piece. As someone who helps families wrongly accused of SBS and Rickets, this is very good information, too bad we cant force every prosecutor and judge to read it.
Some more current research is available here: http://www.familylawweek.co.uk/site.aspx?i=ed56598
Beyond all the scientific evidence, which the average rocket scientist wouldn’t understand, babies can subject themselves to these forces by jumping in a Jumperoo or Jolly Jumper.
Hundreds of videos now are on YouTube of nannys caught on nannycams shaking babies, and none of these babies have ever demonstrated even one of the Triad described as SBS????
In every single prosecution, nobody has ever been caught shaking a baby where that baby had the Triad????
It has never been scientifically proven that it is even possible to shake a baby to death by shaking alone????
In a few cases I know of where people had plead guilty to SBS, all were grieving fathers, all had been given a plea bargain, plead guilty and we will give your other children to your wife and you will get out in a year.
Why are most of the deaths between 4 and 6 months and why are these babies dying only days after vaccination????
Why is it that when a baby dies in hospital of the Triad, that the COD is SIDS, but if it occurs at home it is SBS????
SBS is the worst kind of junk science, it involves accusing grieving parents, often before their child dies. The Crown Prosecution Service in the UK no longer use the term SBS due to so many cases being overturned on appeal, but they still use the same junk science under a different name, NAHI.
Recent tests with CRABI by Dr John LLoyd, a Biomechanist have proven that a baby old enough to use a Jumperoo can generate the forces supposedly necessary to shear the bridging veins. This is the ONLY scientific study EVER conducted on a human baby (who is now 5 years old and shook himself in his Jumperoo).
Unfortunately Medical Science has degenerated into a religion based on faith and most doctors who accuse parents don’t keep up to date with current medical practice. Time to start prosecuting doctors for practicing outside their area of expertise and destroying the lives of grieving parents.
Thanks again for this piece!
Justin J. McShane says:
Thank you for your kind words and points of reference to additional resources. I agree that SBS allegations are some of the least scientific in the world. Thank you for all that you do for justice.